PSA
How PSA testing added 16 years to my lifespan (so far)
ABOUT PSA
The Urologist in me finds it hard to believe that I have never written a post about PSA, although there has been so much hype about it for the past 20 years!
A usable -a very helpful- tool
This is one more case of a perfectly usable tool causing trouble for those folks who have never heard of, or don’t understand, the basic principles of due diligence and are too inconfident to use a fragile tool well.
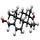
Briefly, the Prostate Specific Antigen (PSA) test is a measure of a prostatic enzyme, PSA, whose physiologic purpose is to liquify the sperm “clot” which forms in the vault of the vagina following ejaculation, thus freeing the Spermatozoa to swim on up to the ovum.
The PSA enzyme is secreted into tiny tubules in the tissue of the prostate and is squeezed out into the ejaculate by spasmodic contraction of the microscopic muscles in the gland, at orgasm.
PSA does not enter the blood, normally
It does not enter the blood, except in tiny quantity, when the prostate is healthy and sexual activity is “normal” (I’ll leave the interpretation of that maltreated word, to the reader!).
However the walls ot the tubules into which the PSA enzyme is secreted are only one cell thick and ANY damage to the tubule wall can result in leakage into the interstitial fluid surrounding the tubule, whence it enters the blood.
Caveat
I must emphasise that in the case of the intra-prostatic tubules, “ANY DAMAGE” translates to “ANY DISTURBANCE”, because the walls are so thin........ Any undue pressure in, or on, the prostatic tissue can produce such leakage.
UNBEKOMING, the substack blogger, is correct
So you are correct, Unbekoming, in saying (I quote from your post) “An elevated reading — typically above 4.0 ng/mL — does not mean you have cancer. It means your PSA is above an arbitrary threshold that was never scientifically validated. Enlarged prostates, infections, recent ejaculation, cycling, and even the digital rectal exam itself can elevate PSA. Three out of four men with elevated PSA do not have cancer” .............
My “take” on PSA
I would list the Causes of elevated PSA, thus - pessure on the prostatic tubules, by:
Pressure rise due to abdominal straining, from constipation,
Rectal examination by the Urologist,
Prostatic massage by a foreign body, such as during same-sex encounters,
Coitus and ejaculation,
Straining at the urine, in cases of Benign enlargement of the gland (BPH),
Riding a bicycle, in the presence of BPH,
Prostate infection, whether from sexually transmitted disease, or urine infection
Masturbation.
CANCER OF THE PROSTATE.
Protocol for the PSA test
In view of these caveats,
The ordering physician should ensure that venipuncture for the test is performed at a time when none of the above factors is in effect:
Interpretation of the results MUST be the prerogative of a practising Urologist, who ensures that confounding factors are absent and repeats the test, to ensure its veracity.
A test is never interpreted on the basis of a single estimation – it is always repeated, after a short interval if positive, or a long time later, if “suspicious”: emphatically, no solo test result is interpreted as an indication of Prostate cancer or even as a reason for prostate biopsy, without being confirmed by repetition
(the suspicious finding is a rise, in the PSA level, from a previous test).A confirmed positive test is an indication for ultrasound or MRI imaging of the gland, but the diagnosis of “Ca Pr” can only be based on examination of a specimen of prostate tissue by a pathologist.
NOTE: I fail to understand the claim that the PSA test leads to “overdiagnosis”, because no diagnosis is made on the basis of the test and even a positive, biopsy-proven diagnosis does not automatically lead to radical surgery: the situation is always assessed carefully by a Urologist. In any case, mild disease is managed on a “watchful waiting” basis and the choice of surgery as therapy depends on many carefully-considered factors, including the patient’s preference.
My Opinion
To jettison a test which can provide early warning of a fatal cancer, citing a high incidence of surgical complications, is a direct affront to the competent surgeon: bear in mind that the complication rate involved in this particularly challenging surgery varies markedly from surgeon, to surgeon ................ Let me explain, via an anecdote:
The operation which is currently in vogue, radical, nerve-sparing retropubic prostatectomy, was developed by Dr. Patrick C. Walsh, Urologist, of Johns Hopkins Hospital, in 1983. His anatomically correct, retropubic approach dramatically reduced rates of postoperative impotence, but From a technical point of view, the precision required for this operation is greater than can be achieved by some surgeons and even in his hands, low-grade incontinence of urine proved to be a problem: his success vis-a-vis urine leakage was not guaranteed (a technique he used, to prevent late post-surgery blockage from scarring, was giving some trouble).
I saw Dr Walsh’s paper on RPP in 1984
I became aware of Dr Walsh’s technique in 1984 and immediately, realising its superiority in terms of both surgical difficulty and liability to postoperative complications, I began to perform it in the Fall of that year.
I chose candidates for the procedure very carefully (at the time I was not particularly busy): I did only one or two per year and by the end of 1991 I had done only 16 cases.
My results were good in terms of success in nerve-sparing, for postoperative sexual function and maintenance of urinary continence, but in 16 cases, I had had 16 minor, inconsequential but annoying surgical hurdles to clear.
I went to watch Dr. Walsh operate
So I called Dr Walsh and asked whether I might be allowed to visit Johns Hopkins Hospital, to observe his technique – he made me welcome and one sunny Tuesday, I watched him do two RPP surgeries (he was doing four RPPs per week - about 200 per year - he had already done more than 800 RPP operations).
I mimicked his technique
Returning to Toronto, I mimicked Dr Walsh’s technique precisely, with instantly excellent results: I performed 84 more RPPs between 1992 and 1997, with no further minor complications. My success rate, vis-a-vis urinary continence was 90-95% (actually better than Dr Walsh’s, from that single point of view) and vis-a-vis postoperative erectile function, was close to 90%, as compared to Dr Walsh’s personal assurance of 94+%. The U. of Toronto Hospitals admitted a success rate of 40%.
A really difficult procedure, requiring precise technique
The point here is that in terms of difficulty, RPP is challenged only by brain surgery and heart transplant. – Therefore in the hands of a neophyte, or a less-than-adequate surgeon, “UNBEKOMING” may be correct in his opinion e. PSA, but I can assure you that a thinking, logical, dextrous surgeon should not find it difficult, to decipher the admitted conundrum of PSA, select the surgical candidates wisely and perform the necessary surgery without incident or mishap.
I had Prostate Cancer, diagnosed in 1994
ONE MORE ANECDOTE: I am a 30-year Prostate Cancer survivor. I went back to see Dr Walsh in 1994, with my own PSA-diagnosed CaPr.
He removed it that December, with no untoward sequelae.
My PSA has been zero, since and I thank God that I was savvy enough to begin monitoring it as soon as the FDA approved it, in 1986!
Notes from AI, verbatim
A. Surgeon - level factors (dominant variable)
Toronto academic centers have:
High - volume prostate cancer surgeons
Established nerve-sparing expertise
Access to perioperative penile-rehabilitation programs (I’m not familiar with this)
This alone pushes expected EF (Erectile Function) outcomes toward the upper end of global RRP ranges.
B. Patient-level factors
The strongest predictors of EF recovery after RRP are:
Age
Baseline erectile function
Vascular/metabolic comorbidities
Smoking
Bilateral vs unilateral nerve-sparing
Tumor location relative to neurovascular bundles
These variables can swing EF recovery from 10% to 70%.
C. Technique-level factors
By 2025:
Robotic prostatectomy dominates Toronto academic centers
Open RRP is still performed but is no longer the majority
Outcomes for open RRP are slightly less favorable on average, but expert-level open nerve- -sparing can match robotic outcomes in selected cases
Evidence-anchored E F ranges (global, 2020–2024) across high-volume centers:
Toronto 2025 — Expected EF recovery after open bilateral nerve sparing RRP is:
40–60% recovery of erections sufficient for intercourse at 12–24 months
Higher (55–70%) in ideal younger, healthy patients
Lower (10–35%) in older or comorbid patients
CONCLUSION
It is unsurprising, in view of the relatively poor results of RPP surgery generally, that those attempting it are so pessinistic about their success rates that they hesitate to diagnose, let alone offer surgery for, Ca Pr.
But put it this way: if I had not started testing in 1986 and if I had not “followed-up” on the slight uptick in my PSA in 1994, I would have died in 2010.
At a reasonable estimate, therefore, by checking my PSA, then referring myself to a really good surgeon, I have thus far added 16 years to my life.


Really appreciated this reading. The hardest part about PSA screening is that it’s neither “always do it” nor “never do it”; it’s a risk-stratified, values-based decision.
From a physician-scientist lens, the most helpful framing for readers is:
1. PSA is a risk signal, not a diagnosis.
2. The goal is to detect clinically meaningful cancers early while minimizing harms from overdiagnosis/overtreatment.
3. Context matters: age, family history, ancestry, urinary symptoms, prior PSA trajectory, and (increasingly) tools like repeat PSA, %free PSA, PSA density/velocity, mpMRI, and targeted biopsy to reduce unnecessary procedures.
Thanks for translating a polarizing topic into something decision-quality and patient-centered!
Also, thank you for sharing this and congratulations on being cancer free for 30 years! I hope it helps other men and that good information is not censored.